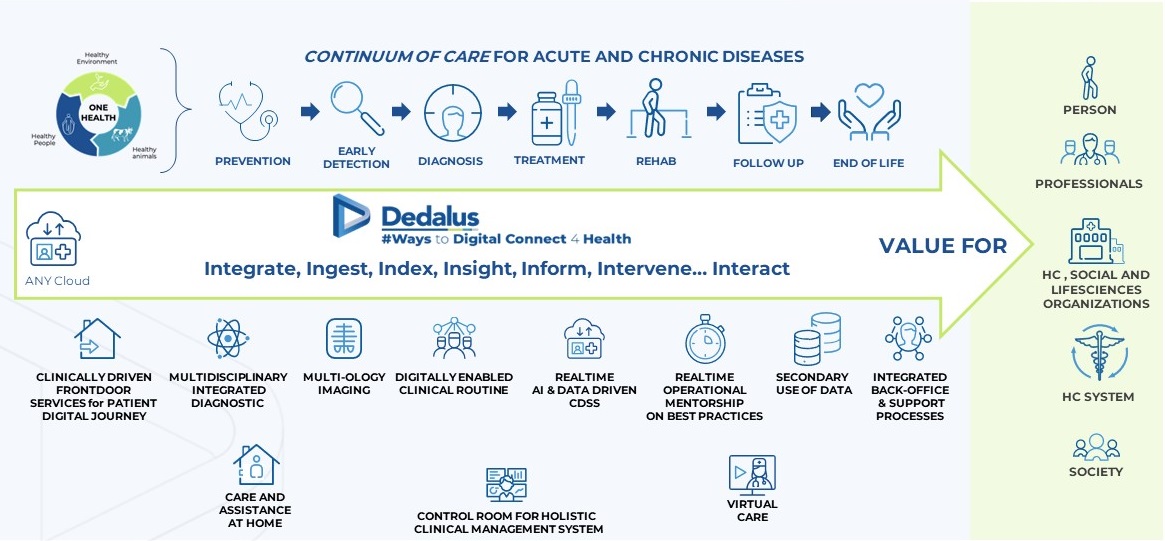
Powering the Whole Person Care Model
Request a brochure, book a demo or simply ask a question: our specialists are available to handle all your needs.

What is Whole Person Care?
In a world with an aging population, an increase in chronic diseases and complex migratory flows, the care model based on “episodes” is no longer applicable. It is imperative to move towards a complete and effective continuum of care paradigm, with the ability to support consumers, caregivers, and social institutions in managing the complexity of the collaboration now required to deliver care.
The Dedalus Whole Person Care Model is a comprehensive healthcare approach focusing on the whole individual. This model recognizes that a person’s physical health is intricately connected to their mental, emotional, and social well-being, and that addressing all these aspects of a person’s life is necessary for overall health and happiness.
How We Achieve Whole Person Care
One of the key elements of the Whole Person Care Model is a strong focus on preventative care. By identifying and addressing potential health risks before they become serious problems, healthcare providers can help individuals maintain their health and avoid future costly medical procedures. This care approach is beneficial for the individual and more cost-effective for the healthcare system.
Another important aspect of the Whole Person Care Model is the emphasis on collaboration and partnerships between healthcare providers, community organizations, businesses, and government entities. Dedalus recognizes that addressing the health needs of individuals cannot be done by healthcare providers alone and that a collaborative approach is necessary to create meaningful and lasting change.
In this innovative approach, the role of Information Technology is essential: enabling the effective and efficient flow of information across multiple settings to ensure the best outcome in each phase: from prevention to early detection, diagnosis to treatment and rehabilitation to follow-up. Individuals, caregivers and health professionals are aware of the overall pathway and contribute effectively to the outcome.
Dedalus offers multiple and diverse solutions for each phase of the continuum of care, ensuring the integration of every care setting, institution, and system in the process.
Key Benefits
- Personalize care and improve patient satisfaction with a holistic approach to whole person care orchestration
- Optimize the use of resources to deliver physical, behavioral, emotional, and social services to improve care coordination and health outcomes
- Amplify the reach of your Care Coordinators and Care Managers
Key Features
- Reduce staff burdens with automated workflows for interventions
- Reduce per capita cost with automated workflows driving patient interventions
- Reduce the rate of hospitalizations with early intervention
- Involve patient’s family and friends to enhance patient well being
- Data at your fingertips with dynamic visualizations to spot abnormal data points
Key Elements of The Whole Person Integrated Care Model:
| Element | Description |
Personalized Care |
Addressing the physical, mental, and social needs of an individual to provide comprehensive and effective care that improves overall well-being. |
Preventative Care |
Identifying potential health risks and addressing them before they become serious problems to maintain health and avoid costly medical procedures. |
Collaboration and Partnerships |
Emphasizing partnerships and collaboration between healthcare providers, community organizations, businesses, and government entities to create meaningful and lasting change. |
Individuals with special needs too often experience poorly coordinated health and social services. The MAC at Morgan’s Wonderland has created a unique whole person care model to orchestrate medical, behavioral and community services for individuals with special needs of all ages, enabled by one connected care software solution.
Dedalus, Microsoft and RxHealth have provided a Personalized Care solution that enables Individual Care Plans, Activity Management, Scheduling, and frictionless Referral orchestration in one integrated, coordinated, mobile platform. Integrated with provider EMRs and SDoH data sources through the Dedalus Connected Care Platform, this end-to-end solution gives care navigators, care teams and individuals with special needs, along with their family members, everything they need to ensure high quality, personalized whole-person care.
.
A: Personalized whole-person care addresses the physical, mental, and social needs of an individual, treating the whole person rather than just a specific medical condition. This type of care is tailored to the individual’s unique needs and circumstances and involves coordinating services from multiple healthcare providers including doctors, nurses, therapists, social workers, and other specialists. This plan includes traditional medical treatments like counseling, therapy, and support groups to address emotional and social issues. The goal of personalized whole-person care is to provide comprehensive, coordinated and effective care that improves the overall well-being of the individual.
A: Dedalus provides a Personalized Care solution enabling individual care plans, activity management, scheduling, and referral orchestration in one integrated, coordinated, mobile platform. The Dedalus Connected Care Platform is integrated with provider EMRs and SDoH data sources giving care teams everything they need to ensure high quality, personalized whole-person care.
A: Personalized whole-person care leads to improved overall well-being, better management of chronic conditions, and a reduction in unnecessary healthcare utilization.
A: Social determinants of health (SDOH) refers to the social and economic factors that impact a person’s health and well-being. These factors include access to education, food, income, housing, and transportation. Whole-person considers a person’s social needs to provide comprehensive and effective care.
A: Integrating whole person care with an electronic health record (EHR) system can involve several steps, including:
- Identifying the specific needs of the whole person care program: This may include identifying the types of data that need to be collected and shared among different healthcare providers, such as information on social determinants of health, behavioral health, and functional status.
- Mapping the data elements of the EHR to the whole person care program: This may include identifying the specific fields in the EHR that will be used to collect and store data related to the whole person care program, and making sure that these fields are easily accessible to all relevant healthcare providers.
- Creating workflows and care pathways: This may include developing care pathways that guide patients through the whole person care program, and creating workflows that help healthcare providers collaborate and share information.
- Interoperability: Integrating the EHR system with other systems, such as telehealth, remote monitoring devices, and other digital health tools that can support the whole person care program.
- Training and education: Providing training and education for healthcare providers on how to use the EHR system to support whole person care, and also educate patients on how to access and use the system.
- Continual monitoring and improvement: Regularly monitoring the use and effectiveness of the EHR system in supporting whole person care and making necessary adjustments to improve the care experience.
By implementing these steps, the EHR system can be used to support whole person care by providing a comprehensive view of the patient, enabling care coordination, and improving communication among healthcare providers.
In conclusion, the Whole Person Integrated Care Model is a comprehensive and innovative approach to healthcare that recognizes the importance of addressing a person’s entire life, including their physical, mental, emotional, and social well-being. By focusing on preventative care, collaboration, and personalized care plans, the Dedalus Whole Person Integrated Care Model has the potential to improve the health and happiness of individuals, while also making the healthcare system more cost-effective and efficient.